Indice del volumen Volume index
Comité Editorial Editorial Board
Comité Científico Scientific Committee
DISSEMINATE CYSTICERCOSIS.
One-day treatment in a case
Foyaca-Sibat H, Ibanez-Valdes LdeF, Mashiyi MK
University of Transkei. Faculty of Health Sciences. Department of Neurology and Department of Internal Medicine.
Nelson Mandela Academic Hospital. Umtata, South Africa.
Rev Electron Biomed / Electron J Biomed 2004;3:39-43.
Comment of the reviewer Sanjib Kumar Sharma MD. Associate Professor, Department of Medicine. BP Koirala Institute of Health Sciences, Dharan, Nepal.
Comment of the reviewer Prof. José María Eiros Bouza. MD. PhD Profesor Titular de Microbiología de la Facultad de Medicina de la Universidad de Valladolid. Espańa.
Key Words: Subcutaneous Cysticercosis, Neurocysticercosis (NCC), Epilepsy, One-day treatment praziquantel
ABSTRACT
We report a patient presenting disseminated cysticercosis characterized by neurocysticercosis, subcutaneous, muscular, and cardiac cysticercosis treated with praziquantel during one day
RESUMEN:
Se comenta el caso de un paciente que presentó cisticercosis diseminada, caracterizada por neurocisticercosis, y cisticercosis subcutánea, muscular y cardiaca, tratada con praziquantel durante un dia.
INTRODUCTION
Neurocisticercosis (NCC) is a parasitic infection of central nervous system (CNS) caused by the larval stage (Cysticercus cellulosae) of the pig tapeworm Taenia solium. This is the most common helminthes to produce CNS infection in human being. The occurrence of acquired epilepsy or the syndrome of raised intracranial pressure in a person living in or visiting a region where taeniasis is endemic or even in one living in close contact with people who have taeniasis should suggest a diagnosis of cysticercosis; the NCC may remain asymptomatic for months to years and sometimes its diagnosis is made incidentally when neuroimaging is performed. Symptoms and signs are related both to the parasite, and to the inflammatory-inmunological response of the host. NCC is the most common cause of acquired epilepsy worldwide and most of the patients taking phenytoin or carbamazepine for a proper control of their seizures, respond very well.
For interested peoples, other aspects concerning to NCC from our region are available on line 1-4 Disseminate presentations of this parasitic disease are not common in our region, only one patient was previously reported by Bhigjee and Sanyika in 19995. Typical manifestation are subcutaneous cyst present as nodules that tend to be asymptomatic. The natural history of the infection remains unknown up to date however is well known that most cysticercus complete their development within 2 to 4 months after larval entry living there months to years, and their locations in order of frequency are the central nervous system, subcutaneous tissues, striated muscle, eyeball, heart, and other tissues.
Human cysticercosis is acquired after eating food contaminated with fertilized eggs excreted in the faces of Taenia carriers, as is also well known that people eating infected pork meat acquire taeniosis no cysticercosis. In humans the most common routes of infection (cysticercosis) are ingestion of T solium eggs from contamined food and rarely from fecal-oral auto-infestation from patients harbouring the adult parasite in their intestines. While the cysts can develop in any human tissue, they have a predilection for CNS. The aim of this study is to report our clinical findings in a patient presenting disseminated cysticercosis and his response to one-day treatment with praziquantel (ODTP). To our knowledge, this is the first report about disseminated cysticercosis treated with ODTP.
Case Report
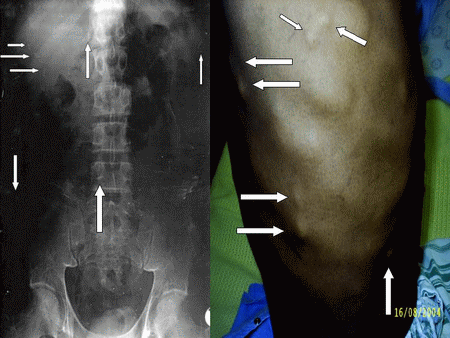
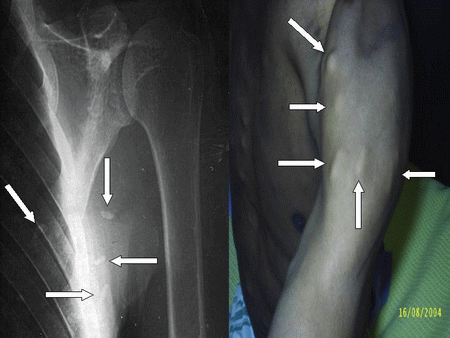
A 42-year-old man admitted at Nelson Mandela Academic Hospital (Umtata) South Africa presented with a history of recurrent generalized tonic-clonic epileptic seizures of six years duration, disseminated nodules all over the body of two-year duration and headache. On general examination multiple subcutaneous and intramuscularly, mobile, no tender nodules, measuring from 0.7 to 2.5 cms, were palpable on the chest, back, abdomen, and proximal regions of the four limbs. (Figure 1-2-3) Respiratory and Cardiovascular system were normal except for a bradicardia of 42 bpm. A detailed neurological examination revealed unremarkable findings.
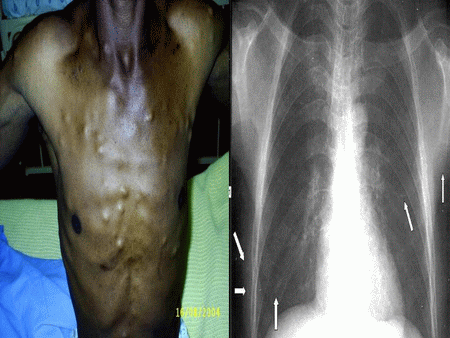
Figure 1: Multiple subcutaneous nodules on the chest wall and a few calcified lesions on chest X-ray
Laboratory data included routine blood test (FBC, U&E, glucose, urinalysis) were normal, erythrocyte sedimentation rate and cardiac enzymes were also normal. ELISA test and IgG for cysticercosis were strongly positive. ECG and cardiac ultrasound confirmed: sinus bradicardia, II grade heart block, and calcifications in papillary muscles and upper septum respectively. CT Scan of the brain showed bilateral cysts in different stages and calcified NCC (Figure 4).
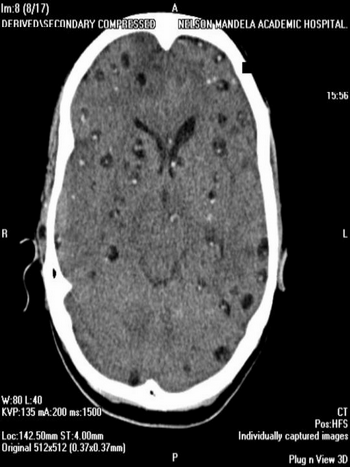
Figure 4: CT Scan of the brain shows: Multiple cysts in vesicular, (scolex inside the cyst are well identified) some cysts in colloidal stage surrounded by perilesional edema, and scanty calcified lesions on both cerebral hemisphere.
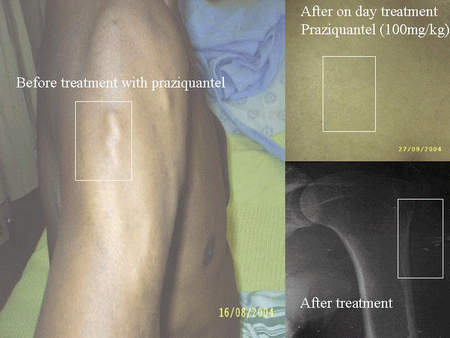
Patient was on 400 mg of phenytoin orally at bed times and he remained free of seizures for several months before came back to neurocysticercosis clinic complaining of recurrent seizures, and radiographic examinations revealed multiple calcified lesions on the chest, abdomen, and four limbs, in many places those calcifications did not coincide with corresponding position of the nodular lesion (Figure 1-2-3) then a diagnosis of active cysticercosis was done and patient was treated with ODTP orally. After of 4 doses of praziquantel (25mg/kg each) two hours interval in one single day treatment some of the subcutaneous nodular lesions disappeared (Figure 5) but the patient began to complain of muscular pain on the proximal regions of the four limbs and fever of six days duration, at this time creatine kinase in serum was also normal.
ODTP caused remarkable changes on the radiographic features of the CT brain Scan but few active lesions were still present therefore two weeks later this patient was treated with 800 mg daily Albendazole and 40 mg of prednisone orally for a week and next CT Scan did not show active cysts only few calcified lesions.
Discussion
Clinical Diagnosis
Diagnostic criteria for disseminated cysticercosis are based on the presence of NCC, subcutaneous (represent cysticerci in the skin), and muscular cysticercosis simultaneously. Unfortunately, little have been published on the medical literature about disseminate cysticercosis. China has the higher prevalence of subcutaneous cysticercosis worldwide probable because there also has the largest population but scanty report about disseminated cysticercosis from there provide limited information. Due to that lack of studies of correlation NCC-SC its percentage of occurrence is also ignored.
Investigations
Ultrasography to diagnose subcutaneous cysticercosis was introduced by Gupta et al6recently but they found some limitations to differentiated cysticercotic lesion from lymphadenopathies, neurofibromas, and epidermoid cysts, however we identified calcified subcutaneous nodules by plain X-rays studies, and positive serological test for cysticercosis supported our diagnosis, and changes observed on the nodular lesions after ODTP should be convincible but biopsy of the skin nodules with pathological examination is the investigation of choice for final diagnosis. CT Scan of the brain is better than MRI for a diagnosis of calcified NCC.
Treatment
Disseminated cysticercosis treated with praziquantel is not a novel event, Wadia et al7 in 1988, reported their results for the first time to the medical literature and ten years later Takayanagui and Chimelli 8reported a patient with an associated diffuse myalgia, fever, and normal creatine kinase level caused by degenerating cysts, similar situation in our patient was also observed. Maxillofacial cystcercosis is an uncommon appearance of a common disease reported recently9 however most of the patients presenting SC remain free of symptoms therefore we suggest anti-parasitic medication when there is clinical manifestation related to location of the nodular lesions or for cosmetic purposes; anti-parasitic treatment for "interruption" of the life cycle of Taenia solium does not has sense because practice of cannibalism have been eradicated and risk of propagation of this type of infection by eating human flesh is not certain. Nevertheless, ODTP should not be indicated until active cysticercosis on the heart is ruled out. We really do not know about additional damage on the cardiac muscle; branches of the coronary arteries or conduction system of the heart caused during parasite’s dying process after treatment with praziquantel. There is not enough accumulated experience about treatment with praziquantel for myocardial involvement in disseminated cysticercosis because only one report from Burkina Faso using albendazole has been made10. To prevent more damage than benefits we suggested do not use anti-parasitic treatment is some pathological condition7and cardiac cysticercosis should be considered until further clinical trials proven otherwise. There are not replacements for a better primary health care system and health education, proper sanitation, and better food hygiene, access to safe water and clean water, and alleviation of poverty as a best way for solving this problem.
References
1. - Foyaca SH, Ibańez VLdeF. Clinical trial of praziquantel and prednisone in rural patients with neurocysticercosis presenting recurrent epileptic attacks. The Internet Journal of Neurology 2002;1(2). Available online from:
http://www.ispub.com/ostia/index.php? xmlFilePath=journals/ijn/vol1n2/ncc.xml
2. - Foyaca SH, Ibanez-Valdes LdeF. Intraventricular neurocysticercosis in HIV positive patients. The Internet Journal of Neurology.2003;2(1). Available online from:
http://www.ispub.com/ostia/index.php?xmlFilePath=journals/ijn/vol2n1/ncc.xml
3. - Foyaca S.H, Ibanez V. LdeF. Vascular dementia type Binswanger’s disease in patients with active neurocysticercosis. Electron J Biomed 2002;1:1-12. Available online from:
http://biomed.uninet.edu/2002/n1/foyaca.html
3. - Foyaca SH, Ibanez-Valdes LdeF. Pseudoseizures and Epilepsy in Neurocysticercosis. Electron J Biomed 2003;1(2):79-87. Available online from:
http://www.uninet.edu/biomed/2003/n2/2foyaca.html
4. - Foyaca-Sibat H, Ibanez-Valdes LdeF. Neurocysticercosis in HIV-positive patients. The Internet Journal of Infectious Diseases 2003;2(2):1-10. Available from:
http://www.ispub.com/ostia/index.php?FilePath=Journals/ijid/current.xml
5. - Bhigjee AI Sanyika C. Disseminated Cysticercosis. J Neurol Neursurg Psychiatry 1999;66:655
6. - Grutta R, et al Diagnosis subcutaneous cysticercosis by Ultrasography. Ultrasound Rev 2001;3(1):23-30
7. - Wadia N, Deasi S, Bhat M. Disseminated cysticercosis; new observations, including CT scan finding and experience with treatment by praziquantel. Brain 1988;111:597-614
8. - Takayanagui MO, Chimelli L. Disseminated Muscular Cysticercosis with Myosits Induced by Praziquantel Therapy. Am J Trop Med Hyg 1998;56(6):1002-1003
9. – Sidhu at al. Maxillofacial Cysticercosis: Uncommon Appearance of a Common Disease J Ultrasound Med 2002;21:199-202
10. – Niakara A, Cisse R, Traore A, Niamba PA, Barro F, Kabore J. Myocardial localization of a disseminated cysticercosis. Echocardiographic diagnosis of a case. Arch Mal Coer Vaiss 2002;95(6):606-608
Disseminated Cysticercosis, Neurocysticercosis though
not a uncommon entity, they are less reported. Dr
Foyaca-Sibat et al. illustrated a good case report and
effective treatment with one-day course. However, a
randomized controlled trial on this issue will be most
welcomed.
Comment of the reviewer, Prof. Sanjib Kumar Sharma MD. Associate Professor, Department of Medicine. BP Koirala Institute of Health Sciences, Dharan, Nepal.