Indice del volumen Volume index
Comité Editorial Editorial Board
Comité Científico Scientific Committee
INTERMEDIATE SYNDROME:
A TYPICAL PATTERN OF
PRE-RENAL ACUTE RENAL FAILURE
IN THE ELDERLY
Musso CG, Luque K, Reynaldi J, Pidoux R, Greloni G, Algranati L
Nephrology Department - Hospital Italiano de Buenos Aires. Argentina
- Anatomically, the aged kidney has a reduced number of glomeruli and glomerular capillaries due to the senile glomerulosclerosis process. These histological changes make the aged kidney prone to progress easily to parenchymal damage under stressful situations 8
- A reduced renal defense against hypoperfusion due to dysautonomy, meaning that vascular autoregulation is altered making renal blood flow and the glomerular filtration rate not constant during large changes in renal perfusion pressure2.
- A reduced defense against volume contraction because of the presence of primary hypodipsia, and reduced sodium and water reabsorption capability 9. The reduced sodium reabsorption capability is secondary to an alteration in the reabsorption of this cation in the ascending loop of Henle10, and distal tubules8. Besides, increased plasma atrial factors contribute to urinary sodium excretion10.
The senile reduction in water reabsorption capability is due to the medullary hypotonicity and the altered response to antidiuretic hormone that it produces11.
- Tubular frailty, attributed to the reduced number of mithocondria in their tubular cells. This could signify a reduction in the energetic reserve that tubular cells have in order to resist ischemia9.
Rev Electron Biomed / Electron J Biomed 2004;3:33-35.
Comment of Reviewer Dr. Javer Lavilla. Nephrology Department. Clínica Universitaria. Pamplona. Espańa
Comment of Reviewer David Rush MD. Section of Nephrology, Department of Medicine, University of Manitoba. Winnipeg. Canada
SUMMARY:
Acute renal failure is a frequent entity in the elderly. This is due on one hand to the structural and physiological changes of the aged kidney, and on the other hand to the exposure of this population to polypharmacy and their reduced capability to metabolize drugs.
In the present report we present a case of a seventy year-old woman who developed acute renal failure secondary to severe dehydration with a clinical and laboratory pattern of intermediate syndrome: laboratory results compatible with parenchymal renal insufficiency (elevated urinary sodium, plasma urea and creatinine), but with a positive response to hydration. The main characteristics of the aged kidney that predispose to the development of an intermediate syndrome are: the vascular dysautonomy and reduced capability of sodium and water reabsorption. The intermediate syndrome is a typical pattern of pre-renal insufficiency in the elderly.
RESUMEN:
La insuficiencia renal aguda es frecuente en el anciano. Esto se debe por un lado a los cambios estructurales y funcionales propios del rińón senil, y por otro a la gran exposición que esta población tiene a la polifarmacia, y su reducida capacidad para metabolizar los medicamentos.
En este reporte presentamos el caso de una mujer de 70 ańos que desarrolló una insuficiencia renal aguda secundaria a severa deshidratación, mostrando un patrón clínico y de laboratorio propio de un sindrome intermedio: laboratorios compatibles con una insuficiencia renal parenquimatosa (sodio urinario, uremia y creatininemia elevadas), pero con una respuesta favorable a la hidratación. Las principales características del rińón senil que predisponen al desarrollo del sindrome intermedio: son la disautonomía vascular y la reducida capacidad en la recuperación de sodio y agua El sindrome intermedio es un patrón típico de insuficiencia prerrenal en el anciano.
INTRODUCCIÓN
Acute renal failure is a frequent renal syndrome in the elderly. This phenomenon is due to the morphological and functional renal changes that occur with aging, the exposure of the aged population to polypharmacy and their reduced capability to metabolize drugs 1. In the following case report a typical pattern of pre-renal acute renal failure in the aging population is presented
CASE REPORT:
A 70 year-old woman was admitted to our hospital presenting a confusional syndrome in the context of severe hypernatremia and acute renal failure. On examination, oral and axillary dryness, orthostatism, oliguria, hypotension (blood pressure: 90-50 mmHg) and slight hypothermia (rectal temperature: 36.8°C) were documented.
She was a self-sufficient person, she took no medications and she suffered no diseases.
A week before admission she had started with watery diarrhea that progressively led her to severe dehydration. At the time of her hospital admission she had no more diarrhea but she was still very dehydrated.
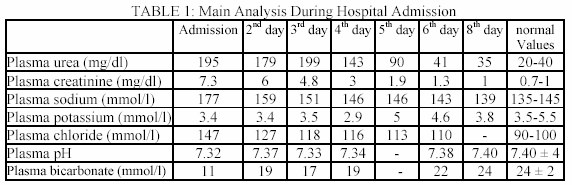
Plasma urea (195 mg/dl), plasma creatinine (7.3 mg/dl), and urinary sodium levels (UNa: 90 mmol/l) were high. Hyperchloremic metabolic acidosis (pH: 7.32 / bicarbonate:11 mmol/l) was also documented. Renal ultrasonography was normal. Blood cultures were taken and water was given by nasojejunal tube, at a rate of three litres per day.
Once rehydration was initiated, neurological status, diuresis, acid-base, plasma sodium, urea and creatinine values improved progressively. Blood cultures were negative.
After eight days of treatment, acute renal failure was resolved normalizing her confusional syndrome and laboratory alterations (Table I).
DISCUSIÓN
Acute renal failure is usually classified in three categories depending on its pathophysiological mechanism 2:
1) Pre-renal insufficiency, in which there is renal hypoperfusion secondary to real or effective hypovolemia: volume depletion, decreased cardiac output, peripheral vasodilatation or redistribution of extracellular fluid.
2) Intrinsic renal insufficiency, in which there is parenchymal damage secondary to prolonged hypoperfusion (ischemia) or renal toxicity2,3.
3) Post-renal insufficiency, in which there is urinary tract obstruction as the pathophysiological mechanism2.
In order to distinguish pre-renal insufficiency from intrinsic renal insufficiency, three parameters are usually considered: clinical examination, laboratory analyses and response to volume expansion2. For instance, if a patient has low urinary sodium, higher plasma urea than plasma creatinine, signs of dehydration and a positive response to volume expansion, he will be diagnosed as having pre-renal insufficiency; while if a patient has urinary casts, high urinary sodium, high plasma urea and creatinine levels, edema, and a negative response to volume expansion, he will be considered to have intrinsic renal insufficiency4,5.
However, a third situation has been described, named intermediate syndrome6. It consists of a patient whose blood and urinary laboratory results seem to be those of intrinsic renal insufficiency (i.e. high plasma urea, creatinine and urinary sodium), but his renal insufficiency gets better with volume expansion, behaving as a pre-renal one. However, the intermediate syndrome ameliorates more slowly than pre-renal insufficiency: its renal function recovery takes more than twenty-four hours, but less than a week. Histologically, intermediate syndrome represents a partial acute tubular necrosis, a situation between the absence of tubular necrosis (pre-renal insufficiency) and its total installation (parenchymal renal insufficiency)6.
Many characteristics of the aging kidney predispose aged people to suffer intermediate syndrome 7:
All the above mentioned factors make the aging kidney capable of developing partial tubular necrosis, and as a consequence a pattern of intermediate syndrome.
The documented hyperchloremic metabolic acidosis was probably due to an alteration in the amoniagenesis process in the context of tubular damage.
CONCLUSION:
Intermediate syndrome is a typical pattern of hypovolemic pre-renal insufficiency in the elderly.
REFERENCES
1) Macías Núńez J, Sanchez Tomero J. Acute renal failure in old people. In Macías Núńez J, Cameron JS (Eds). Renal function and disease in the elderly. London. Butterworths; 1987: 461
2) Faber M, Kupin W, Krishna G, Narins R. The differential diagnosis of acute renal failure. In Lazarus JM, Brenner BM (Eds). Acute renal failure. New York. Churchill Livingstone. 1993:133-139
3) Faber M, Kupin W, Krishna G, Narins R. The differential diagnosis of acute renal failure. In Lazarus JM, Brenner BM (Eds). Acute renal failure. New York. Churchill Livingstone. 1993:147-148
4) Faber M, Kupin W, Krishna G, Narins R. The differential diagnosis of acute renal failure. In Lazarus JM, Brenner BM (Eds). Acute renal failure. New York. Churchill Livingstone. 1993:149-184
5) MillerT, et al. Urinary diagnostic indices in acute renal failure. Annals of Internal Medicine 89: 47, 1978.
6) Chapman A, Legrain M. Acute tubular necrosis and interstitial nephritis. In Hamburger J, Crosnier J, Grunefeld JP (Eds). Nephrology. New York. Wiley-Flammarion. 1979: 383
7) Musso C, Macias Nuńez JF, Mayorga M. ‹Value of urinary sodium in diagnosis of the sort of renal insufficiency in the elderly› Rev Arg Ger Ger 16: 129, 1996
8) Musso C. Geriatric nephrology and the "nephrogeriatric giants". International Urology and nephrology 34:255-256, 2002
9) Macias J, Bonda A, Rodriguez JL. Physiology and disorders of water balance and electrolytes in the elderly. In Macias J, Cameron JS. (Eds). Renal function and disease in the elderly.London. Butterworths.1987: 67-92
10) Musso C, Macias Nuńez. El rińón del anciano: morfología y función. Principales neuropatías. In Salgado A, Guillén F, Ruipérez I (Eds). Manual de Geriatría. Barcelona. Masson. 2002: 401
11) Musso C, Fainstein I, Kaplan R, Galinsky D, Macías Núńez JF. El paciente con transtornos del equilibrio hidroelectrolítico y ácido base. In Macias Nuńez JF, Gullén Llera F, Ribera Casado JM. Geriatría desde el principio. Barcelona. Glosa.2002. 247-248
Comment of reviewer Dr. Javer Lavilla. Servicio de Nefrología. Clínica Universitaria. Pamplona. Espańa
Acute renal failure is a relevant clinical problem in the elderly, since they have worse control of the internal milieu than young people. They have also a reduced functional renal reserve (secondary to a progressive nephronal loss due to the aging process and concomitant diseases such as: diabetes mellitus, hypertension, nephrotoxic drugs, etc.)
Among the main causes of acute renal failure in old ambulatory population, there are absolute hypovolemia (dehydration secondary to fever, diarrhea, etc.), non-imflammatory relative hypovolemia (cardiac failure, hypoxia, etc.) and inflammatory relative hypovolemia (sepsis, etc.).
Others causes of acute renal failure in this group are obstructive uropathy (prostatic disease) and renal parenchymal damage (nephrotoxic drugs, vasculitis, etc.).
In this report a case of an intermediate syndrome is presented. This refers to a renal alteration between a pure pre-renal insufficiency and a complete acute tubular necrosis, and is a frequent pattern especially in patients admitted to hospital, since their renal failure is caused by many variables: sepsis, nephrotoxic drugs (aminoglycoside), etc.
There are helpful markers for detecting renal damage as is urine N-acetylglucosaminidase (proximal tubules), gammaglutamyltranspeptidase (distal tubules), and doppler ultrasound resistance index (nephrotoxic damage secondary to oncologic drugs).
It is very important to point out that rehydration is always the first treatment for any acute renal failure, but one should be cautious with patients suffering from pulmonary distress or restrictive cardiopathy.
Comment of Reviewer David Rush MD. Section of Nephrology, Department of Medicine, University of Manitoba. Winnipeg. Canada
Musso et al. describe correctly the pathophysiological changes suffered by the aged kidney that expose the elderly to develop acute renal failure. It is also important to point out the influence of senile anatomical changes (reduction in kidney size and number of glomeruli, increase in the mesangium area due to a diminution in capillary volume) and reduced metabolization of drugs, on the elderly exposed to acute renal damage.
Received: July 29, 2004. Reviewed: October 26, 2004.
Published: November 3, 2004
