Indice del volumen
Volume index
Comitť Editorial
Editorial Board
Comitť CientŪfico
Scientific Committee
ERYTHEMA NODOSUM AND PROLONGED FEVER ASSOCIATED TO SECONDARY HYPERPARATHYROIDISM
Enz P*, Musso C**, Luque K**, Kowalczuk A*, Galimberti R*, Algranati L**.
Dermatology* and Nephrology** Departments.
Hospital Italiano de Buenos Aires. Argentina
carlos.musso @ hospitalitaliano.org.ar
Rev Electron Biomed / Electron J Biomed 2005;2:67-72
Comment of the reviewer Omar Abboud, MD, FRCP, FRCPE. Consultant Nephrologist. Hamad Medical Corporation. Doha, Qatar.
Comment of the reviewer Antonio Fťlix Conde MartŪn. MD. Pathologist. Hospital Universitario Perpetuo Socorro. Badajoz, Spain.
SUMMARY
Secondary hyperparathyroidism is one of the main deragements caused by chronic renal failure, and parathyroid hormone is considered one of the toxins of the uremic syndrome. Prolonged fever due to primary hyperparathyroidism have already been described in the literature but not yet as induced by secondary hyperparathyroidism. In this case report a patient suffering from an erythema nodosum and prolonged fever associated to secondary hyperparathyroidism that disappeared through subtotal parathyroidectomy is presented.
RESUMEN
El hiperparatiroidismo secundario es uno de los principales disturbios causados por la insuficiencia renal crůnica, y la paratohormona es considerada una de las toxinas del sindrome urťmico. El sindrome febril prolongado secundario a hiperparatiroidismo primario ya ha sido descripto en la literatura, aunque no lo ha sido aun el inducido por hiperparatiroidismo secundario. En el presente reporte se presenta un caso de eritema nodoso y sindrome febril prolongado asociado a hiperparatiroidismo secundario y que resolviů luego de efectuada una paratiroidectomŪa subtotal.
Keywords: Secondary hyperparathyroidism, Erythema nodosum, Prolonged fever
Palabras Clave: Hiperparatiroidismo secundario, eritema nodoso, sindrome febril
INTRODUCTION
Secondary hyperparathyroidism is one of the main deragements caused by chronic renal failure, and elevated plasma parathyroid hormone is considered one of the toxins of the uremic syndrome. Many chronic renal failure problems have been attributed to parathyroid hormone effect such as ureamic cardiopathy, erythropoiesis reduction and inhibition of platelet and T-cell functions1.
Even though prolonged fever due to primary hyperparathyroidism have been already described in the literature, it is infrequent 2, and this entity has not yet been described as induced by secondary hyperparathyroidism. For that reason in the following case report a patient suffering from an erythema nodosum and prolonged fever associated to secondary hyperparathyroidism is presented.
Case Report
Female patient thirty-one years old suffering from chronic renal failure secondary to a vesicoureteral reflux in her childhood. She developed a severe secondary hyperparathyroidism: plasma intact parathohormone 1500 pg/ml (normal value in CRF: 150-300 pg/ml) (Tables 1 and 2).
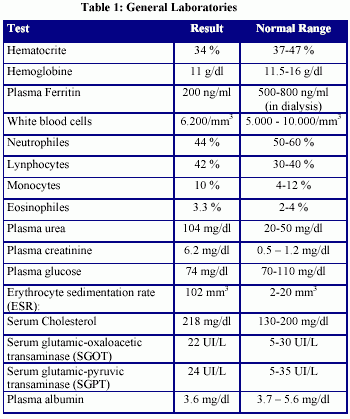
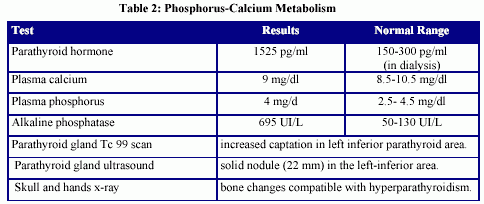
Two months before starting hemodialysis she had begun with fever and an erythema nodosum in the distal and anterior part of her legs (diagnose confirmed through skin biopsy). The fever was vespertine and without chills. The beginning of the dialytic treatment did not modify these symptoms. Many studies were performed in order to roule out infectious, neoplastic or autoimmune diseases. All results were negative or did not justify neither the prolonged fever nor the erythema nodosum (Tables 3, 4 and 5).
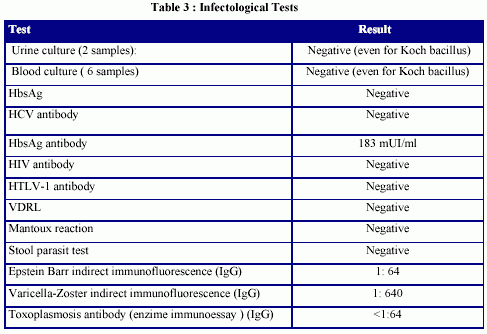

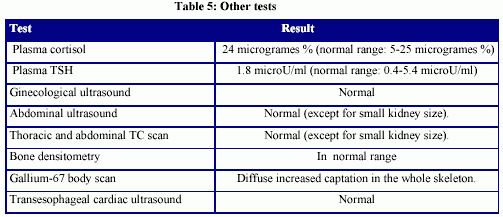
Initially her hyperparathyroidism was treated with phosphorus binders ( calcium carbonate) and intravenous calcitriol but it had to be discontinued many times due to the high plasma phosphorus levels that she developed. Because of that she had to be operated on her parathyroid gland. She was on no medication except for phosphorus binders, acid folic and B vitamin complex.
After that her plasma parathyroid hormone levels normalized and concomitantly the erythema nodosum and febril syndrome did too.
Discussion
Secondary hyperparathyroidism is promoted by several chronic renal failure deragements that generate an increase in plasma parathyroid hormone level, being the most important ones the hypocalcemia, diminished circulating calcitriol levels and phosphate retention 3.
Under normal conditions this hormone stimulates the bone turn-over, but in chronic renal failure is one of the main toxins resposible of the uremic toxicity. Secondary hyperparathyroidism leads to damage in many parenchymas: bones, ligaments, heart, etc. Even more parathyroid hormone interferes the activity of the immunological system for instance inhibiting the T cell function 1.
In this report we described a case in which the patient suffered from prolonged fever in the evenings for a period of five months and only disappeared after her hyperparathyroidism was solved through subtotal parathyroidectomy.
During her febrile syndrome she developed erythematous, tender nodules and plaques, on her pretibial areas. An skin biopsy confirmed the diagnose of erythema nodosum.
Erythema nodosum has been described in four kind of diseases: infectious, pharmacological, neoplastic and autoimmunological ones. Several immunological diseases have been described as generating erythema nodosum such as: bowel immflamatory diseases, sarcoidosis, BehÁet and Sweetīs syndrome. It has not yet been described erythema nodosum induced by hyperparathyroidism 4,5.
Epidemiologically this entity is most frequent between 20 and 30 years of age, being 3 to 6 times more frequent in women than in men6.
Immunological pathogenesis for this cutaneous reaction pattern is widely accepted4,5. Regarding the physiopathology of this disease, the hypothesis of an immunological mechanism is accepted4,5. Erythema nodosum is a type III hypersensitivity reaction (Gell and Coombs classification), mediated by antiboby-antigen deposits. After the exposition of the organism for a determined period to a particular antigen (infectious, autoimmune, neoplastic, farmacological or environmental one) it takes place an antibody-antigen union forming immune complexes which are deposited in some organs such as skin, kidney, lungs, etc. Then, an acute immunological reaction begins through complement cascade and immflamatory citokines activation that leads to the characteristic erythema nodosum skin lesion7.
Our patient was studied in order to roule out the presence of infectious, neoplastic, farmacological or autoimmunological causes of prolonged fever and erythema nodosum, but none of them were found.
In our case parathyroid hormone or some part of its molecule could be the antigen that functioned as the stimulus of the skin immunological reaction. This could also explain the fact that the febrile syndrome and the erythema nodosum appeared in the context of a secondary hyperparathyroidism, and also that the skin lesion lasted beyond the habitual lapse for an idiopatic erythema nodosum (4-6 weeks), and that both manifestations (fever and skin lesion) disappeared after the normalization of plasma parathyroid hormone level due to sub-total parathyroidectomy.
Then we hypothezise that our patient prolonged fever and erythema nodosum could have been associated to secondary hyperparathyroidism.
Conclusion:
Prolonged fever and erythema nodosum seem to be one of the uncommon clinical expressions of the secondary hyperparathyroidism.
REFERENCES
1.- Vanholder R, Ringoir S. The uraemic syndrome. In Cameron S, Davison A, GrŁnfeld JP, Kerr D, Ritz E. Oxford. Oxford University Press. 1992: 1236-1250
2.- Ricci J, Vlasschaert J, Salit I. Prolonged fever asociated with primary hyperparathyroidism. Can Med Assoc J. 1984: 131(5): 459-460
3.- Delmez J, Kaye M. Bone disease. In Daugirdas J, Blake P, Ing T (Eds). Handbook of dialysis. Philadelphia. Lippincott Williams & Wilkins. 2001: 530-547
4.- Mert A, Ozaras R, Tabak F, Pekmezci, Demirkesen C, Ozturk R.Erythema nodosum: an experience of 10 years. Scand J Infect Dis. 2004; 36(6-7): 424-427
5.- Bondi E, Margolis D, Lazarus G. Disorders of subcutaneous tissue. In Feedberg I, Eisen A, Wolff K, Austen F, Goldsmith L, Katz S, Fitzpatrick T. (Eds). Dermatology in general medicine. New York. 1999: 1284-1287.
6.- Requena L, SŠnchez Yust E. Mostly septal panniculitis. J Am Acad Dermatol. 2001; 45: 163-183
7.- Roitt I. Essential immunology. Oxford. Blackwell Scientific Publications. 1994: 326
