Indice del volumen Volume index
Comité Editorial Editorial Board
Comité Científico Scientific Committee
THE PLACENTA INFECTED BY HIV AND HPV
Olivar C. Castejón Sandoval, Angela J. López González
Laboratorio de Microscopia Electrónica. Facultad de Ciencias de la Salud.
Universidad de Carabobo.
Nucleo Aragua. Centro de Investigación y Analisis Docente Asistencial del
Nucleo Aragua.(CIADANA).
Aragua State. Maracay. Venezuela.
olivar.ciadanauc @ gmail.com
Rev Electron Biomed / Electron J Biomed 2013;3:28-35.
RESUMEN:
Antecedentes: La conexion VIH/VPH llega a la placenta mediante la transmision materno-fetal desde un utero infectado. En esta coinfeccion el VPH tiene propiedades epiteliotropicas y citoliticas que puedan causar serias lesiones a la estructura de la vellosidad placentaria a la cual puede además asociarse la actividad de los antivirales.
Objetivo: evaluar las alteraciones morfológicas en vellosidades placentarias de paciente con coinfección VIH/VPH.
Material y Método: Placenta obtenida de embarazada de bajo recursos socioeconómicos, con coinfección VIH/VPH, en 38 semanas de embarazo, sin síntomas de otras enfermedades y nacimiento vivo, analizada por microscopía de luz. Como control se utilizó placenta normal aplicando un protocolo de observación que describe nódulos sincitiales, fibrinoide, edema, fibrosis, calcificación e inmadurez.
Resultados: Vellosidades troncales aparecen con dańos vasculares a nivel del endotelio, capa muscular y tejido que rodea los vasos.Acentuados cambios degenerativos a nivel del sincitio y región estromal fueron observados en los diferentes tipos de vellosidades. Escasa arborización de las vellosidades fue encontrada. Fibrosis, deposición de fibrinoide, e infartos son notorios. Abundan las vellosidades intermedias inmaduras sufriendo degeneración.
Conclusiones: Una desconocida interacción de VIH/VPH ha provocado sobre la estructura de la vellosidad placentaria un efecto superior comparado cuando la actividad viral de cada virus es producida individualmente. Este ataque viral poduce un efecto destructivo muy fuerte sobre la placenta.
PALABRAS CLAVE: Alteraciones morfológicas. Vellosidad placentaria. Coinfección VIH/VPH.
SUMMARY:
Background: The connection HIV/HPV reaches the placenta through the maternal-fetal transmission from an infected uterus. In this connection HPV has epitheliotropic and cytolytic capabilities which can cause severe alterations to the structure of the placental villi associating with the activity of antivirals that can increase the proportion of these lesions.
Objective: To evaluate morphological changes in placental villi of patient with coinfection HIV/HPV.
Material and Method: Placenta obtained of patient with low socioeconomic resources and coinfection HIV/HPV at 38 weeks of pregnancy, without another signs of disease, live newborn, which was analized by Light microscopy. Normal placenta was used as control. A protocol of observation that described syncytial nodules,fibrinoid, edema, fibrosis, calcification and immaturity was used.
Results: Stem villi appeared with vascular damage to the level of endothelium, muscular layer and tissue that surround to the vessels. Severe degenerative changes in the syncytium and stromal region were observed in different types of villi. Arborization of villi was scarcity. Fibrosis, deposition of fibrinoid and infarcts are notorious. Immature intermediate villi were seen abundant and degenerate.
Conclusions: An unknown interaction of HIV/HPV has provoked on the structure of placental villi an effect higher compared when the viral activity of each one virus is produced individually. This viral attack leads to a destructive effect very strong on the placenta.
KEYWORDS: Morphological alterations. Placental villi. Coinfection HIV/HPV
INTRODUCTION
It is known that for women living with HIV, there are additional challenges to consider when diagnosed with HPV (Human papillomavirus).HIV and HPV are sexually tansmitted infections that cause abnormal growth of placental tissue. These virus have come by hematic route to the normal placenta. Women living with HIV tend to have multiple types of HPV which is associate with a greater risk of cervical dysplasia which if left untreated it can turn into cancer.
Nevertheless has been described that placentas affected by HIV are a barrier for the viral transmission without inflammatory response neither lesions 1. Inflammation of placental villi is associate with socioeconomic state of the patient 2 indicating that socioeconomic factor could to be affecting the placental infection in patients very poor.
In HPV infection the macroscopic and histological aspect of the lesions provoked by the virus on the squamous epithelium vary according to the localization and type of virus3. These virus have effect of vacuolization of the cytoplasm in the infected cell as vacuolants agents producing warts in genital region. It cause hyperproliferative lesions in epithelial tissues. The infection by HIV has a cytolitic effect destroying the population of TCD4 lymphocytes and is located in the placenta as mentioned by means of maternal-fetal transmission since the infected uterus during pregnancy. The virus produce, in placental villi, interruptions of syncytial plasmamembrane, edema, loss of ribosomes at level of RER, disappearance of mitochondria, Golgi Complex, RER, lysosomes, cytoplasmic filaments and dissolution of hyaloplasmic matrix. In consecuense a vacuolar image also is observed associated with nuclear fragmentation in stromal cells4.
HIV positive women with severe immunosuppression are 5 times more likely than HIV-negative women to have lower genital tract neoplasias5. Strong and consistent relation between coinfection with HIV / HPV and cervical intraepithelial neoplasia (CIN) has been shown6
HPV types considered to be of high oncogenic risk, as types 16 and 18 are found in nearly all cases of CIN and cervical cancer and can cause persistent infections and such cases can be infected by multiple HPV types5
This HIV/HPV connection could to be provoking in the human placenta degenerative changes in placental villi which has not been evaluated. Immunosuppression in women infected with HIV could so to be a condition in which HPV in placental villi increase his aggressive effect and then to produce severe degenerative changes in the structure of the villi.
The purpose of this study is to demonstrate the morphological changes provoked in placental villi by the presence of a coinfection with HIV/HPV.
MATERIAL AND METHODS
Placenta was obtained of patient of low socioeconomic recourse with coinfection HPV/HIV, at 38 weeks, who had antiretroviral therapy by human acquired immunodeficiency syndrome using protocol of the group of clinical essay of pediatrics AIDS7,PACTG 076 according to sigla in English, indicating 3'Azido3'deoxythymidine(AZT) as Connor et al8 during the third trimester of pregnancy. The placental weight was 570gr and newborn weight of 3060 gr.
Serology of patient was negative for hepatitis B, C, cytomegalovirus, Epstein Barr virus, rubella and toxoplasmosis. Without other metabolic disease, genetic or parasitic, with live newborn and not knowledge of their further development. Informed consent and the approval of the ethical committee of our hospitaler institution for this research was given according to Helsinki declaration. Patient was diagnosed by Micro-Elisa of fourth generation, with automatic equipment AXSYM(Abbot,EUA) and test confirmatory Western Blot Assay HIV Blot 2.2 of MP Diagnostics(Germany-Singapore Science Park). In the laboratory of molecular biologic diagnostic was reconfirmed in fresh material of placental villi with PCR stain.
HPV test, papanicolau test and clinical exam were used for the diagnostic of HPV in woman pregnancy. The placenta was examined with histological slides by light microscopy. 5 biopsy taken from marginal and central region of basal plate were obtained. From each biopsy 5 slides were obtained for H-E stain and 25 slides were seen. A normal placenta without viral infection at same gestational age with similar socioeconomic state of woman pregnancy totally healthful was obtained for to compare. A protocol of observation with 6 variables was used for both placentas which contained syncytial nodules, fibrinoid changes, villous edema, stromal fibrosis, calcification and immaturity villous.
In order to evaluate these lesions 20 camps were taken by each slide with the objective of 40x. These were seen with a photomicroscope MC63A Zeiss, standard clinic(Carl Zeiss, Oberkochen,West Germany) according to morphological criterion of the literature9-10. In such observations the features with more rebound will be taken for microphotography in this descriptive and preliminary study.
RESULTS
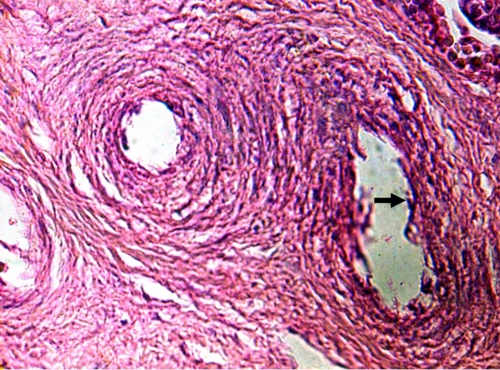
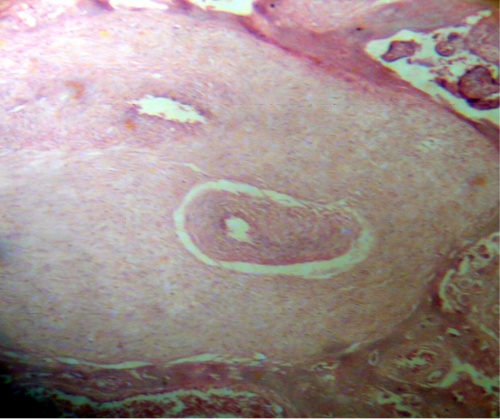
Stem villi were seen with vessels that have an endothelium very spoiled where the cells are separated forming sometimes a net; these vessels are located in an stromal oedematous region (Fig.1). Their muscular layer is observed damaged and the endothelium has disappeared(Fig.2).
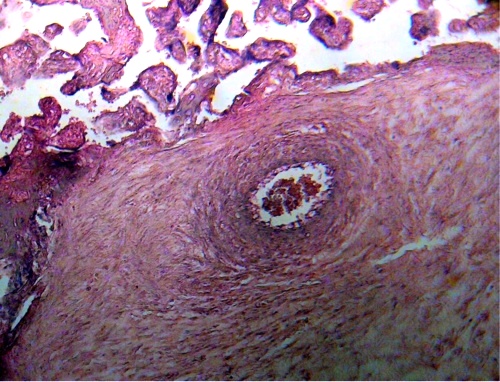
Figure 1.- A zone of stem villi which shows a vessel with damaged endothelium in stromal oedematous region. H-E.160x.
In some stem villi these vessels are totally separated and surrounded by an ring of edema losing their connection with fibers and cells of stromal region (Fig.3). These observations were not seen in control placenta. There are zones where stem villi has lost large part of the structure as interruptions of the syncytium, necrosis of it and disappearance of vessels (Fig.4).
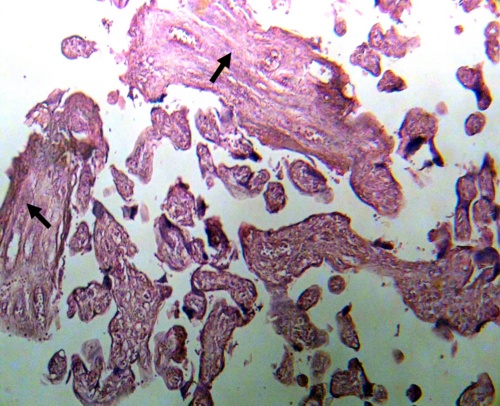
Figure 4.- Severe degenerative changes are seen in stem villi ( Flechas) indicating a viral destructive effect.H-E.160x.
Regions of stromal fibrosis frecuently are found in stem villi (Fig.5).The connection HPV/HIV appear to have a destructive and generalized effect on the structure of the stem villi. This leads to limited arborization. The structure in normal placenta was seen intact. Fibrotic placental villi of different types are observed in regions where also can be seen filiform villi (Fig.6).
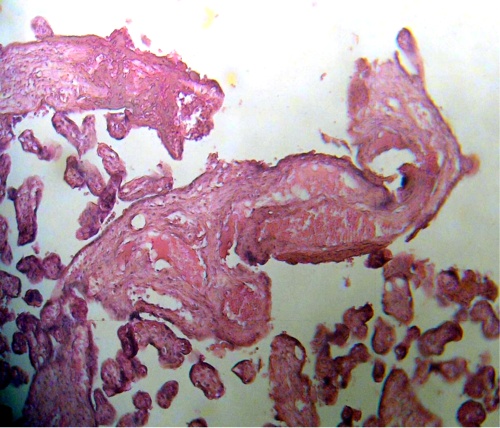
Figure 5.- Stem villi are observed with fibrotic stroma associate to fibrinoid deposition. H-E.160x.
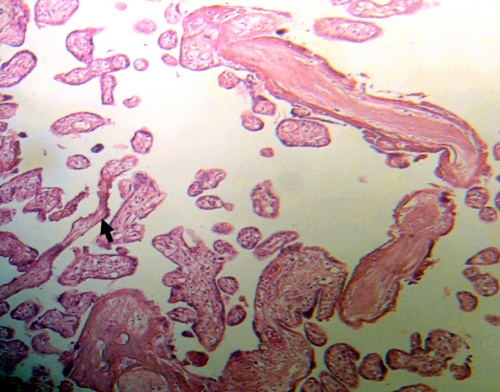
Figure 6.- Numerous fibrotic villi have lost their vessels. Filiform villi is observed (Flecha). H-E.160x.
Numerous villi are affected by a strong deposition of fibrinoid. This is located in the periphery of the villi or in their stromal region associated to the destructive effect of the viral action. Normal stromal region is observed in the control. With frecuency regions of infarcts are seen associated to this deposition of fibrinoid (Fig.7).
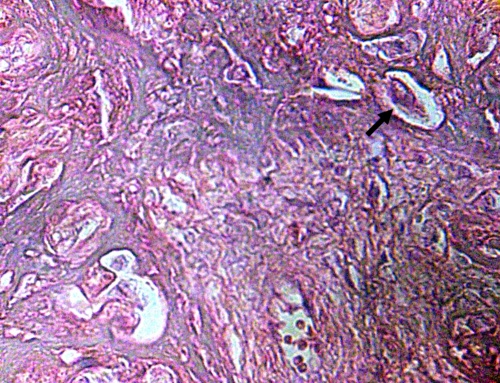
Figure 7.- Zone of infarct with fibrinoid deposition. Figures similar to koilocytes are observed (Flecha). H-E.640x.
Infarcts were found diminished in the control. Immature intermediate villi was found in great proportion when compared with the control. Many villi of this type exhibits a destructive generalized effect with peripheric fibrinoid deposition or in stromal region, without vessels and debris of syncytium (Fig.8) not observed in normal placenta.
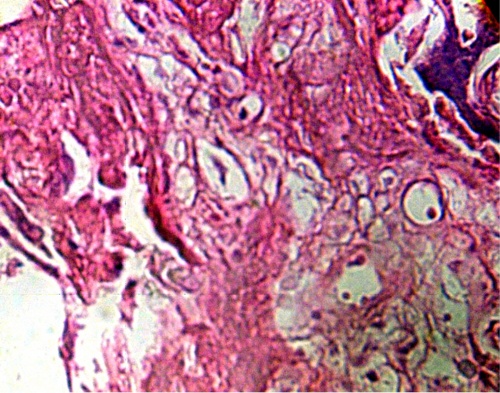
Figure 8.- Region of immature intermediate villi which shows a destructive effect by the connection HPV-HIV. H-E.640x.
DISCUSSION:
HPV is an epitheliotropic virus typically infecting keratinocytes but also possibly epithelial trophoblastic placental cells.HPV infect placental material and is associated with spontaneous abortions in the first and second trimester of gestation11. This virus plays an important pathogenetic role since high risk types are associated with cancer. The lesions are characterized by presence of koilocytes with irregular hyperchromatic nuclei surrounded by a perinuclear cytoplasmic clear halo as observed in figure 7.
Endothelial and muscular damage of the layers of vessels in an oedematous stromal region also have been seen in cases of presumably congenital cytomegalovirus infection (CMV)9 although with associate vasculitis which could not be seen by us. The edema that separate the vessel could facilitate their collapse diminishing the blood flow. The no inflammatory response in this work has also been seen in congenital herpes infection9.
Destructive effect, extensive obliterative fetal vascular damage, intravellous hemosiderin deposition and villitis can be seen in infectious disorders of the placenta with rubella, CMV and herpes simple10. In our case fibrinoid deposition was seen probably in their immunological significance of protective function9. Fibrinoid contains molecules that provides immunoprotection as heparan sulfate proteoglycan12. Fibrinoid acts as an immunoabsorptive sponge containing immune complexes in which the viral activity would be neutralized13.The connection HPV/HIV has provoked a process of placental immaturity which is expressed in an increasing population of immature intermediate villi. These types of villi were seen in this work notably affected for this viral connection.
Morphological changes were observed in placentas with VIH as deposits of fibrin, intervillous thrombosis and infarcts in the intervillous space. Besides congestion vascular, intraluminal calcification and changes in the muscular layer of blood vessels which were found in a higher percentage when compared with normal placentas14. There are significative differences between placentas of patients infected by VIH and normal placentas with respect to cyncytial nodules, fibrinoid changes, edema, calcification and villous immaturity(15).The cytopatic effect of this virus on the placental villi has been confirmed by an ultrastructural study in villi treated with zidovudine4. At difference of the hystopathological features of the lesions found in these last studies the presence of this viral combination has provoked a higher attack to the structure of the villi. An increased net of fibrinoid deposition in the stromal region associate to running plasma when sincitio is interrumpted appear to provoke a crack in the placental villi as seen in figure 8. In our case we have seen greater aggressiveness. We not know how this viral connection produce this notable viral aggression.HPV appears to increase the aggressive effect of the VIH, in a condition similar to the occurred in patients with VIH where HPV increase the risk of neoplasia16.
Complex interactions between HPV and HIV have been described. HPV and VIH each display interactions favoring the other infection to cellular level. The reciprocal enhancement of viral replication leads to worsened patients with HIV as their immunity lowers. The interactions start at the molecular then at the cellular level, allowing each infection favor the acquisition and the amplification on the other one17. This then translates into a higher aggressiveness of the HPV in patients with HIV due to progressive immunosuppression. It is unlikely that each virus interact directly or physically in a sustained manner.HPV infected cells regulate HIV expression and HIV is associated with the expression of HPV genes18. This aggressive course of HPV infection in HIV-positive women has been reflected in increased HPV loads predictive of cervical cancer19.
In conclusion, an unknown interaction of HPV and HIV on the structure of placental villi has provoked severe degeneratives changes with a higher effect compared when the activity viral of each virus is produced individually. This increased attack produces a strong destructive effect on the placenta.
REFERENCES
1.- Jauniaux E, Nessmann C, Imbert MC, Meuris S, Puisant F, Hustin J. Morphological aspects of the placenta of HIV pregnancies. Placenta 1988;9:633-642.
2.- Loga FM, Driscoll SG, Munro HN. Comparison of placental villi from two socioeconomic groups.I.Morphometry.Pediatrics 1972;50:24-31.
3.- Kasper DL, Braunwald E, Fauci AS, Hauser SL, Longo DL, Jameson JL. Harrinson.Principios de Medicina Interna. 16a edicion. Mexico:Mc Graw Hill,2006.
4.- Castejon OC, Lopez GAJ, Castejon MOC. Ultrastructural aspects of the HIV-1 infection in human placental villi with zidovudine treatment.Ginecol Obstet Mex 2010;78:335-344.
5.- Ferenczy A, Coutlee F, Franco E,Hankins C. Human papillomavirus and HIV coinfection and the risk of neoplasias of the lower genital tract: a review of recent developments.CMAJ 2003;169:431-434.
6.- Wright TC, Ellerbrock TV, Chiasson MA,Van Devanter N, Sun XW. Cervical intraepithelial neoplasia in women infected wth human immunodeficiency virus: prevalence, risk factors and validity of papanicolau smears. New York cervical disease study. Obstet Ginecol 1994;84:591-597.
7.- Bulterys M. HIV during pregnancy preventing vertical HIV transmission in the year 2000: Progress and prospects-A review. Trophoblast Research 2001;15:S5-S12.
8.- Connor EM,Sperting RS, Gelber R, Kiselev P, Scott G, O' Sullivan MJ et al. Reduction of maternal-infant transmission of human immunodeficiency virus type-1 with zidovudine treatment. N Engl J Med 1994;331:1173-1180.
9.- Benirschke K, Kaufmann P. Pathology of the human placenta 4ta Ed. New York: Springer-Verlag,2000.
10.- Lewis SH, Perrin E. Pathology of the human placenta . 2Ed. New York: Churchill Livingstone,1999.
11.- Weyn C, Thomas D, Jani J,Guizani M, Donner C, Van Rysselberge et al.Evidence of human papillomavirus in the placenta. J Infect Dis 2011;20:341-343.
12.- Kisalus LL, Herr JC. Immunocytochemical localization of heparan sulfate proteoglycan in human decidual cell seretory bodies and placental fibrinoid. Biol Reprod 1988; 39:419-430.
13.- Swinburne LM. Leucocyte antigens and placental sponge. Lancet 1970;2:592-593.
14.- Castejon S OC. Alteraciones morfologicas en el espacio intervelloso y en los vasos de vellosidades troncales de embarazadas infectadas con VIH tratadas con zidovudina.Rev Elect Portales Medicos.com 2009;4:442-449.
15.- Castejon SOC, Lopez GAJ, Perez YLM, Castejon MOC. Lesiones de la vellosidad placentaria en pacientes con infección por VIH-1 tratadas con zidovudina. Ginecol Obstet Mex 2011;79:269-279.
16.- Lefevre J, Hankins C, Money D, Rachlis A, Pourrreax K,The Canadian Women'S HIV study group et al. Human papillomavirus type 16 viral load is higher in human immunodeficiency virus-seropositive women with high-grade squamous intraepithelial lesions than in those with normal cytology smears. J Clin Microbiol 2004;4:2212-2215.
17.- Konopnicki D, De Wit S, Chumeck N. HPV and HIV coinfection. A complex interaction resulting in epidemiological, clinical and therapeutic implications. Future Virology 2013;8:903-915.
18.- Sisay S, Erku W, Belay M, Sisay Z, Tiruneh M, Woldeyohannes D .Efffect of human papillomavirus HIV infected person. A mini review. Internat J Med Sci 2013;3:351-356.
19.- Weissenborn SJ, Funke AM,Hellmich M, Mallmann P, Fuchs PG, Pfister HJ et al. Oncogenic human papillomavirus DNA loads in human immunodeficiency virus positive women with high grade cervical lesions are strongly elevated. J Clin Microbiol 2003;41:2763-2767.
ACKNOWLEDGEMENTS
To the administrative direction of the Health Sciences Faculty of the Carabobo University Aragua Nucleus by institutional fixed funds for the CIADANA. To the personnel of the Obstetric and Ginecol department of the Central Hospital of Maracay Aragua by facilitate the placenta with clinic history. To Aragua Fundacite by financial support in part for this research.
CORRESPONDENCE:
Prof. Olivar C Castejón.
Laboratorio de Microscopia Electrónica.
Facultad de Ciencias de la Salud.
Universidad de Carbobo.
Nucleo Aragua.
Centro de Investigación y Analisis Docente Asistencial del Nucleo Aragua.(CIADANA)
Maracay. Venezuela.
Apdo. 4944.
olivar.ciadanauc @ gmail.com